A child in Canada diagnosed with leukemia has an approximately 90 percent chance of survival, but in the world’s poorest nations, 90 percent of such children die of the disease. This disparity was at the heart of a symposium on global cancer care held Saturday at the Dana-Farber Cancer Institute and co-sponsored by two Harvard-based programs, the Global Oncology (GO) initiative and Students for Global Oncology. Cancer is not just a problem of the developed world, emphasized researchers and clinicians from across the Harvard community, and in lectures, panels, and small-group discussions, speakers considered the unique challenges the disease poses in the countries least equipped to treat it.
The problems of global oncology are largely those that plague healthcare across the developing world. There is little awareness of cancer and its causes, so patients are diagnosed late and may face stigma when seeking treatment. Chemotherapy requires frequent and sustained therapy that is often interrupted when drugs run out or are slow to arrive, and simply reaching a doctor can be a struggle for the many people who live in rural areas, far from the nearest clinic. These barriers—not to mention the often-prohibitive cost of treatment—are daunting, even though more than half of new cancer cases occur in low- and middle-income countries, along with nearly two-thirds of cancer-related deaths.
“There’s lots of room for what we can do before we reach what we can’t,” said Felicia Marie Knaul, Ph.D. ’95, an associate professor at Harvard Medical School and director of the Harvard Global Equity Initiative (HGEI), a research program studying equitable development. In the developing world, she and other speakers emphasized, many of the new cases are preventable. Tobacco is the main culprit; public-health initiatives have cut smoking in wealthier nations, but it continues to cause lung and other cancers worldwide. Viral infections are major factors as well. Hepatitis B virus (HBV) can cause liver cancer and human papilloma virus (HPV) cervical cancer; both can be prevented using vaccines. Such prevention is relatively inexpensive—HBV vaccines in particular now cost well under $1 per dose—but the virus’s tolls remain high. According to the World Health Organization, the trio of HBV, HPV, and hepatitis C virus still cause an estimated 20 percent of cancer-related deaths in low- and middle-income countries.
Even in the case of treatment, speakers argued, progress need not be prohibitively expensive. Much of the world lacks access to relatively inexpensive, generic drugs, and detecting cancers earlier would make such treatments more effective. Improvements are also tied to broader institutional progress. In particular, said Knaul, “We can ride the wave of universal health coverage.” According to an HGEI report she coauthored, 30-month survival for childhood cancers has increased from approximately 30 percent to nearly 70 percent under Mexico’s universal health initiative, Seguro Popular. (Knaul witnessed the initiative’s implementation firsthand: her husband, Julio Frenk, current dean of the Harvard School of Public Health (HSPH), designed the program as minister of health, and Knaul, who was diagnosed with breast cancer in 2007, has experienced the country’s health system as a patient as well. She has founded a nonprofit organization to promote breast cancer research and awareness in Latin America and written a memoir about her experiences.)
Simultaneously, Thomas Gross, deputy director of the National Cancer Institute Center for Global Health, emphasized a need for public-health strategies tailored to available resources. “High-income countries should resist the temptation to focus on exporting the latest, most expensive technologies,” he said, “and focus on partnering with countries to develop resource-appropriate strategies to decrease their burden and mortality.” He quoted Theodore Roosevelt: “Do what you can, with what you have, where you are.”
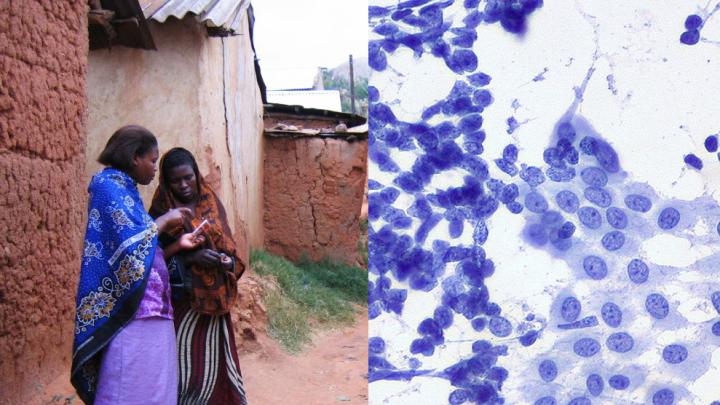
At the same time, the developing world presents unique biological challenges, which were the subject of a GO-sponsored lecture held in the fall semester. “Cancer just looks different in Uganda,” said Corey Casper, director of the program in global oncology at the Fred Hutchinson Cancer Research Center. In his collaborations with the Uganda Cancer Institute, he often encountered cancers like Kaposi’s sarcoma and non-Hodgkin’s lymphoma that are infrequent in the developed world but common in Africa, where they develop almost exclusively together with HIV. Exactly how HIV contributes to these cancers’ development is still unclear. The subject is rarely studied in the developed world, Casper said, but understanding the particularities of these HIV-associated cancers might be necessary to develop effective treatments.
Saturday’s symposium concluded with a call to action. Rifat Atun, professor of global health systems at the Harvard School of Public Health, described lessons from the worldwide effort that has curbed the incidence of HIV and made it a more manageable, chronic illness; cancer, he said, could be tackled using the same commitment and ambition. Kolokotrones University Professor and Partners in Health co-founder Paul Farmer, the closing speaker, framed global oncology as part of a broader struggle against unequal access to healthcare. Against concerns expressed about the cost of public-health interventions, he cited examples like the diminished cost of drugs and vaccines in the wake of government investments—and argued that the economics of healthcare could be altered by societal commitments. “We should fix our aspirations to global health equity,” he said, emphasizing the moral imperative of action. “The goal is equity of chance and diminishment of risk—trying to do right by everybody.”
Videos from the Global Oncology symposium are available online.